Targeted Complement Inhibition
SUMMARY
In many autoimmune diseases as well as in transplant rejection, antibodies bind to host tissues and trigger activation of the complement system leading to severe organ damage. The complement system is obviously not there to damage organs but is providing essential protection against infections and mediates tissue homeostasis. This aspect makes therapeutic complement inhibition challenging as strong complement inhibition will result in infectious risk and a dysregulated homeostasis. There are currently a few complement inhibitors on the market, but these inhibitors work systemically, indicating that throughout the body complement is inhibited while the complement activation and tissue damage can be highly localized to one tissue or even one cell type. In addition these drugs are extremely expensive, highly limiting their use. We have developed strategies to target complement inhibition to specific tissues / cells to achieve local complement inhibition while leaving the systemic complement pool available to fight infections and achieve homeostasis.
BACKGROUND
Current treatments for autoimmune diseases and transplantation typically involve (systemic) immunosuppression. In addition, in several diseases where a clear and essential role for complement was observed, complement inhibitors are employed. These complement inhibitors do inhibit complement effectively, however, they require high dosing and come with a risk for infections and with extreme costs. While many more diseases would be eligible for complement inhibitory treatment this is currently not seriously contemplated as it will not outweigh the risks or the costs. By achieving localized complement inhibition with long lasting inhibitors one could circumvent the downsides of current technologies and open up possibilities for many more clinical conditions that can benefit from a localized and short term complement inhibition. So far the only method to achieve local complement inhibition in humans has been local injection in the eye. Clearly not the most sophisticated way to achieve such inhibition and not applicable to other target organs / tissues frequently affected by complement mediated damage.
TECHNOLOGY
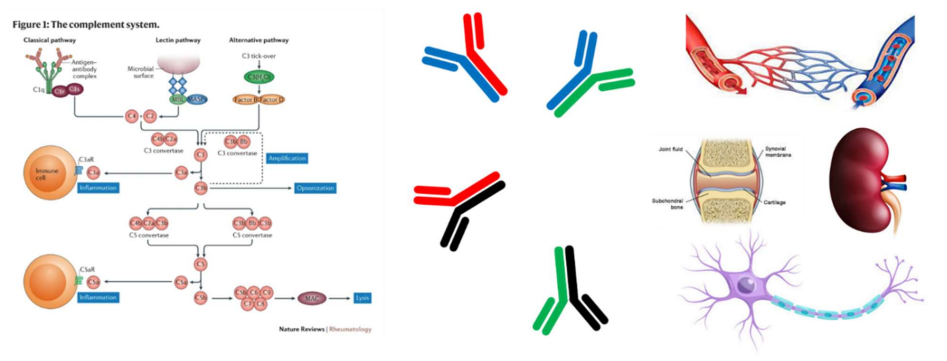
The invention builds on the use of bi-specific antibodies that allow targeting of a specific tissue or cell type and provides local complement inhibition on that target. The modular nature of these bi-specifics allows for a wide range of targets to be selected and allows for a inhibition of the classical and lectin pathway or the alternative pathway, or all three.
VALUE PROPOSITION
The complement-targeted therapeutics market is expected to strengthen its roots in the global market at a strong CAGR of 22.9% between 2022 and 2032 (www.futuremarketinsights.com).
TEAM
Dr. Leendert Trouw currently holds a position as Associate professor at the department of Immunology at the Leiden University Medical Center in Leiden/ The Netherlands.
Key benefits
- Local instead of systemic complement inhibition avoids the risk of infections.
- Fully human nonimmunogenic inhibitors compatible with many autoimmune diseases and transplantation.
-Long acting complement inhibitors restore physiological control of complement activation.
Applications
- Applicable to a wide range of autoimmune diseases, cardiovascular disease, metabolic syndrome and transplantation.
- The current invention may also be used to pre-treat organs prior to transplantation.
- Potential to target also non-orphan diseases as the risk profile is much more favorable. Relatively easy to develop as it is built on well-known antibody technology.
Luris reference number
MC00745Patent status
This technology is subject of a patent application (Dutch Patent Application No 2032398).



